Update Jan 2025
The content continues to undergo review by all our cadres.
The content remains subject to the following provisos:
- The content will be subject to continuous update and review
- Old content (from previous CGOs) will be converted into the new format, using the new tools and layouts
- Content may be moved around
- The layout will change and reflect the needs of the user
- Content will be created
- Content may be deleted/retired
CGO development will continue.
Saf
[Updated 21 Jan 2025]
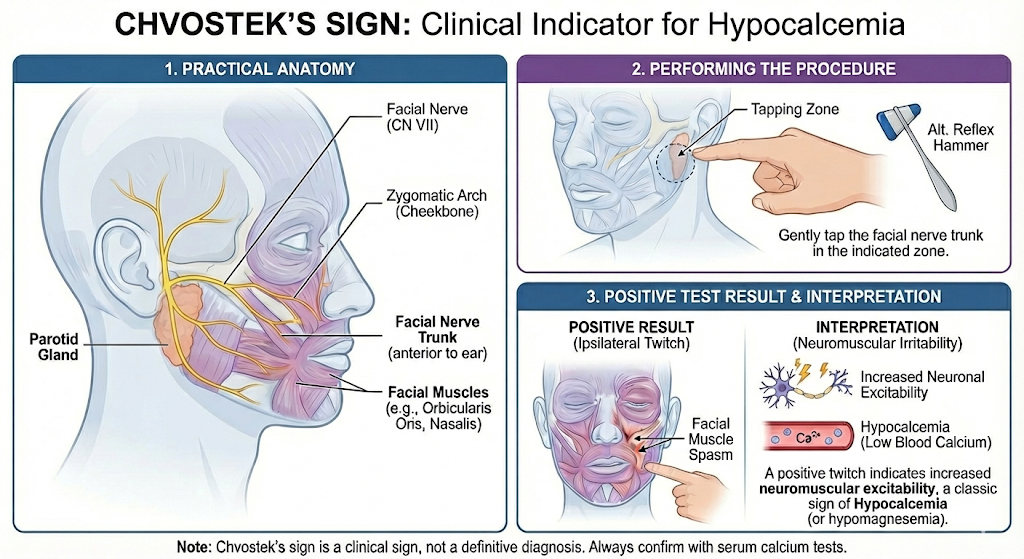
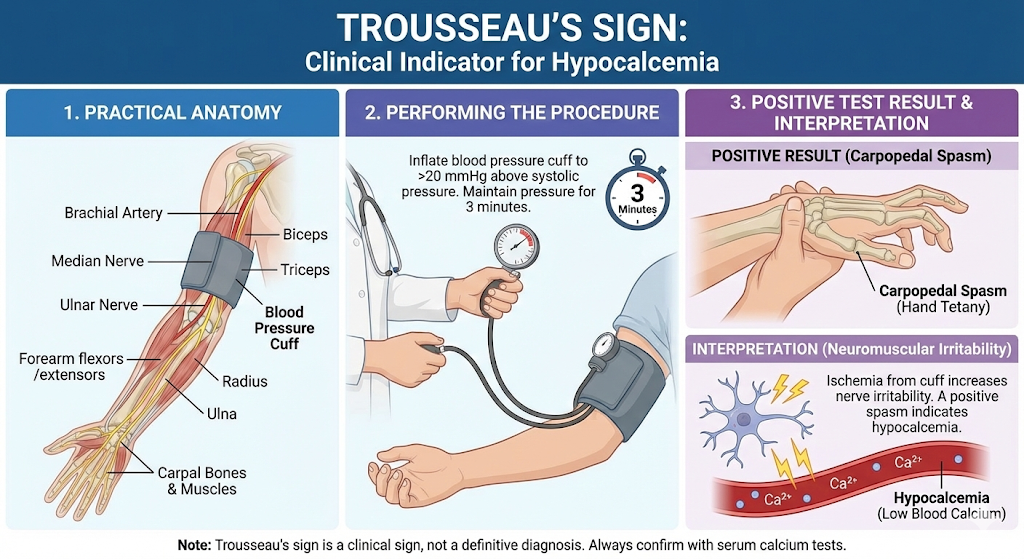
Guide the safe management of deranged calcium levels on Ops
Deployed care of high and low calcium
Clinical decision makers R1 -R3
Symptoms usually develop when adj calcium <1.9mmol/L (ionised <0.9 mmol/L)
Clinical features: are more severe if calcium fall is rapid
Check adjusted serum calcium level. Normal range ionised 1.16–1.31 mmol/L (adjusted serum level 2.1-2.6 mmol/L
Is ionised calcium <0.9 (Adj serum <1.9) mmol/L - OR - Ionised >0.9 (adj serum >1.9) mmol/L AND signs/ symptoms of hypocalcaemia?
YES - Calcium chloride 10% in 10mL. Calcium chloride should be given by large bore peripheral IV, with monitoring for extravasation, or central line if available. If time, to reduce hot flushes, bradycardia, hypotension or arrhythmias, 5ml of calcium chloride 10% can be diluted into 100ml 0.9% saline and infused over 10min with ECG monitoring.
Monitor serum calcium levels every 1-2 hours. In symptomatic patients a continuous infusion is often needed to prevent recurrence.
Assess cause:
Investigations: (where available)
Ionized calcium (iStat) above normal range usually warrants treatment. Accuracy of ionised calcium to distinguish ‘high’ from ‘very high’ is not known. As soon as possible, obtain lab calcium (serum calcium, albumin, U&Es).
ECG – shortened QT interval and dysrhythmias indicative of severe hypercalcaemia
Treatment:
Rehydrate: IV 0.9% saline 4-6L in 24hrs repeat fluids and continue monitoring
Refer to next role.
Second line – seek specialist input:

